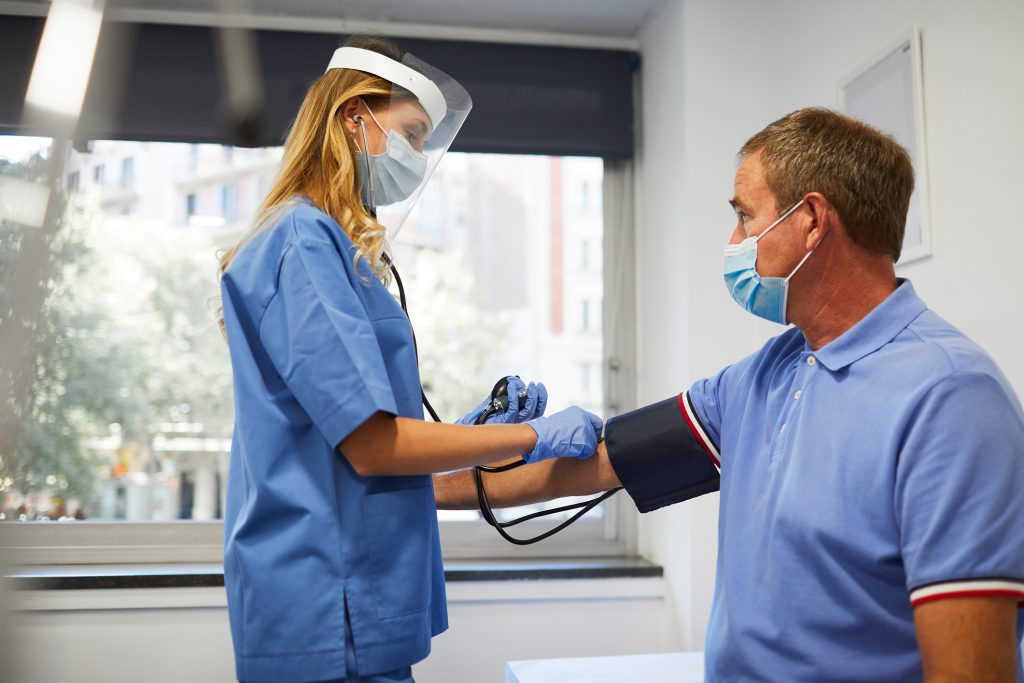
Vital signs are measurements of essential body functions. Part of a physical exam provides a quick and objective way to assess a patient’s health. Taking our vital signs is a simple and speedy procedure we often take for granted without realizing its importance. But for medical assistants and practical nurses, the process has greater significance. Straightforward yet complex, it’s the foundation of quality care.
What Are the Different Vital Signs Medical Professionals Take?
There are four primary and several secondary vital signs. Primary vital signs are the most essential. They include:
Body Temperature
Body temperature is a strong indicator of overall health. Normal readings between 97.8 to 99 °F suggest that the body’s internal environment functions appropriately. Fever indicates an immune or inflammatory response.
Pulse
Pulse is the number of heartbeats per minute. A direct reflection of heart function, an average adult rate of 60-100 beats per minute (bpm) indicates a working circulatory system. High or low readings point to a range of conditions, from anxiety to cardiovascular issues. Notes should also include an assessment of pulse characteristics, including strength, rhythm, and regularity.
Respiratory Rate
The respiratory rate is the number of breaths taken per minute. Average values range from 12-20. Patients may, however, unintentionally alter their breathing patterns if they’re aware their respirations are being monitored.
Blood Pressure
Blood pressure is the force of blood exerted against artery walls. It’s a fundamental reflection of systemic health affecting most major organ systems. Hypertension is a risk factor for heart and kidney disease. Hypotension can lead to fainting, making it a safety concern.
Secondary vital signs are additional assessments that provide a more holistic view of a patient’s condition. Examples are:
Height and Weight
Height and height are used to calculate medication dosages and assess long-term health risks associated with obesity or malnutrition. Sudden changes can also indicate disease.
Pulse Oximetry
Pulse oximetry measures oxygen content in the bloodstream. While not yet considered a primary vital sign, it’s increasingly considered a must-have measurement for cardiac or pulmonary patients.
Level of Consciousness
Level of Consciousness (LOC) is an essential part of neurological exams. Evaluated using the Glasgow Coma Scale, it reflects a patient’s cognitive status and brain function.
Pain Level
Pain level is a subjective measure of comfort. It can, however, affect primary vital signs, so knowing if a patient is in pain helps doctors interpret irregular readings.
Blood Glucose
Monitoring blood glucose levels is essential for patients with diabetes. However, with the higher levels of obesity prevalent in modern society, routine screening for hyperglycemia among the general population is fast becoming the standard. Most practices check it using a glucometer and a fingerstick blood sample.
Capillary Refill Time (CRT)
Capillary refill time is how quickly blood returns to the capillaries after the skin, nail beds, or mucus membranes are compressed. A normal CRT of 3 seconds or less shows circulation is brisk.
Why Are Vital Signs Important?
Vital signs are among a medical professional’s most valuable assessment tools. They play a leading role in patient care for several significant reasons:
Health Assessment
Changes in vital signs can indicate underlying health issues long before symptoms appear. Early detection helps identify risk factors for chronic conditions, such as hypertension, heart disease, and diabetes.
Diagnosis
Many health conditions cause similar symptoms. Doctors must hunt for clues to narrow down the potential cause. Changes in vital signs and other findings can point physicians in the right direction, resulting in a faster diagnosis and quicker care.
Triage
Medical professionals prioritize patients based on the urgency of their conditions. But outward appearances can be deceiving. In a busy emergency room, patients with the least stable vital signs are usually the sickest and are treated first.
Making Treatment Decisions
Vital signs are essential for monitoring the progression of illness and the patient’s response to treatment. Readings show whether a patient is better, worse, or stable, influencing treatment decisions.
Safety Considerations
Vital signs assess health and fitness, ensuring individuals can safely tolerate activity or medical procedures. School sports physicals, for example, may help detect dangerous heart rate abnormalities in children.
Calculating Medication Dosages
Some medications affect vital signs, causing unwanted side effects. Others, such as blood pressure medications, are routinely adjusted based on their impact.
Research
Vital signs are often analyzed to gain insights into health issues. Only by collecting data, for example, were researchers able to correlate high blood pressure to heart disease risk.
What Do Medical Assistants Need to Know About Vital Signs?
How vital signs are approached, obtained, monitored, utilized, and reported can vary significantly based on a medical professional’s role. Medical assistants should know:
Which Vital Signs to Take
Medical assistants focus on primary vital signs, plus height, weight, pain level, and oxygen saturation. Level of consciousness and capillary refill time rarely apply in outpatient settings.
Normal Ranges and Variations
Medical assistants should know the normal ranges for vital signs in their age groups. There are wide variations between newborns and seniors.
Factors Affecting Vital Signs
Age, gender, physical fitness, environmental temperature, and stress level may affect vital signs, providing perspective on abnormal results.
Measurement Techniques
There’s more than one way to take vital signs. Medical assistants should be familiar with the most common techniques and their indications, such as using a temporal thermometer instead of a tympanic thermometer for a child with a history of ear infections; scar tissue can affect the reading.
And while most medical offices have digital vital sign equipment, technology can fail. Some tools, such as digital sphygmomanometers, are less precise than manual measurement methods.
Equipment Limitations
All vital sign equipment has parameters. Cuff fit, for example, is critical for accurate blood pressure readings. And digital thermometers may have upper and lower limits that result in errors if exceeded. Medical assistants must understand the proper use and limitations of their tools.
Safety Considerations
Vital sign equipment can carry germs. It’s essential to sanitize thermometers, blood pressure cuffs, and other devices as directed.
There are also contraindications and precautions to consider. Blood pressure, for example, should never be taken on a limb with a vascular access port. Cutting off circulation, even momentarily, can impair fragile devices.
Interpretation and Recordkeeping Protocols
Interpreting vital signs is beyond a medical assistant’s scope of practice, but they should be able to recognize significant abnormalities requiring follow-up. Results should be noted in the patient’s chart using universal language and approved abbreviations with notes explaining any concerns, such as an elevated pulse in an anxious patient.
What Do LPNs Need to Know About Vital Signs?
Taking vital signs is an essential but routine task for medical assistants. Practical nurses, however, perform clinical assessments, so it has greater significance. An LPN should know:
The Indications for Vital Signs
Monitoring vital signs in acute care settings can help detect life-threatening conditions like infection and respiratory failure. Nurses must know which vital signs to take when symptoms emerge and why. Examples include checking oxygen saturation for shortness of breath and temperature for body aches.
Advanced Measurement Methods
Medical assistants work with stable patients, so there are fewer variations in the vital sign process. However, an LPN may care for a dozen or more patients simultaneously, each with a particular need or a potential contraindication. LPNs should be more familiar with the many options available for taking vital signs and the best specialized techniques for some patients.
Nurses will also rely more on CRT, pain, and level of consciousness assessments to gauge their patient’s conditions. Prolonged CRT in a critical care environment can be an early sign of circulatory collapse requiring immediate intervention, while any decrease in consciousness requires immediate evaluation. Pain, while not always an indication of a worsening issue, impacts the patient’s care plan. A post-surgical therapy session, for example, may need to be postponed for 10/10 pain.
How to Make Treatment Decisions
LPNs are trained to make limited clinical decisions related to vital signs. An LPN can’t prescribe treatment, but they can, for example, activate standing emergency orders for oxygen based on shortness of breath and low oxygen saturation. They may also withhold medications that could harm patients pending a doctor’s review, such as delaying insulin administration for a patient with hypoglycemia.
Nurses must, however, be aware of their scope of practice and legal responsibilities when making clinical calls. Deviating from physicians’ orders should always be a stop-gap measure.
Documentation Requirements
Vital sign documentation goes beyond numbers for nurses. Their notes should indicate whether critical signs were a routine or an acute intervention and why. Evidence of follow-up with a physician or supervising RN is paramount. Notes should identify abnormal vital signs and which nursing actions were taken in response.
Professional Communication and Collaboration
LPNs work closely with physicians, RNs, and other healthcare professionals. Effective communication regarding vital signs and patient status is essential for continuity of care. Treatments may change rapidly in acute care settings, so abnormal results should be noted and passed on verbally to other physicians. For example, a patient with a sudden fever may require immediate infection control precautions affecting all caregivers.
Continuing Education Considerations
Vital sign ranges and methodologies change over time. Best practices are updated based on research findings. Nursing is an evidence-based profession, so LPNs should stay abreast of developments that affect how they take and interpret vital signs. Professional literature is often the best source of information.
Final Thoughts
Modern medicine is a miracle. Still, with all the technological advancements available, the simplest assessment methods are often the best. Vital signs tell a definitive tale that brings context to an often complex clinical picture. As a medical assistant or LPN, you’ll help write happy endings.
Medical Assistant Program
Ready to start a new career as a medical assistant? Gwinnett Colleges & Institute offers medical assisting courses to gain essential skills and training at multiple campuses from Lilburn, Roswell, and Atlanta/Marietta to Orlando, FL, and Raleigh, NC. The core curriculum at these campuses focuses on the medical assisting skills and training you will need to seek entry-level employment in physicians’ offices, clinics, hospitals, and other medical settings needing the services of associates trained in both front and back-office medical assisting skills. These medical assisting courses will be the first step in starting a rewarding career.
Practical Nursing Program
Are you looking for Practical Nursing training classes in Central Florida that prepare you to become a licensed practical nurse (LPN)? Gwinnett Institute in Orlando offers a Practical Nursing diploma program that trains LPN students for positions delivering basic bedside care to patients. The Practical Nursing diploma program provides the didactic and skills training needed to take the NCLEX-PN examination.*
*While Gwinnett Institute provides test preparation and review assistance to college students, it cannot guarantee any college student will be able to take or pass any type of licensure exam. College students must be mindful throughout their training program that licensure is a prerequisite for employment as a nurse and diligently prepare themselves to meet this important requirement.
Contact us today to learn more about becoming an LPN or Medical Assistant at Gwinnett Colleges & Institute.